The process of spermatogenesis, i.e., the formation of sperms, is an essential part of reproduction in humans and all kinds of animals. In this article, we will learn about where and when spermatogenesis occurs, and what are the stages that the cells need to go through to complete the process.
Did You Know?
In humans, spermatogenic cells need to be maintained at around 2°C below the body temperature to function. This is done by the regulation of blood flow and the positioning of the muscles, which keeps the scrotum away from the heat of the body.
Spermatogenesis can be defined as ‘the process occurring in the male gonad of sexually reproducing organisms, wherein the undifferentiated male germ cells develop into spermatocytes, which then transform into spermatozoa’. Spermatozoa are mature male gametes that are present in organisms which are sexually reproductive, and it is similar to oogenesis in females. Spermatogenesis usually occurs in the seminiferous tubules of the testes in a series of stages, followed by maturation in the epididymis, where they become ready to be passed out as semen along with other glandular secretions. This process begins at puberty due to the actions of the hypothalamus, pituitary gland, and Leydig cells, and the process only ends at death. However, the quantity of sperms reduces gradually with age, eventually leading to infertility.
Purpose of Spermatogenesis
The purpose of spermatogenesis is to create mature male gametes, which can effectively fertilize female gametes in order to form a single-celled organism called a zygote, which eventually leads to cell division and multiplication to form a fetus. Also, to have a healthy offspring, the number of chromosomes must be maintained at a fixed number across the body, for which, failure can lead to abnormalities such as Klinefelter’s syndrome, Down’s syndrome, or abortion of the fetus. Spermatogenesis works to avoid this.
Process of Spermatogenesis
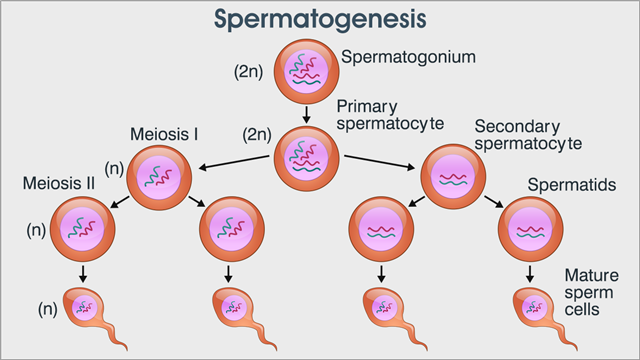
The process of spermatogenesis is very similar in animals and humans. Let us look at each stage of the spermatogenesis process in some detail.
- Stage 1: The original diploid spermatogonium located in the seminiferous tubules has twice the number of chromosomes, which replicate mitotically in interphase before meiosis 1 to form 46 pairs of sister chromatids.
- Stage 2: The chromatids exchange genetic information by the process of synapsis, before dividing through meiosis into haploid spermatocytes.
- Stage 3: In the second meiosis division, the two new daughter cells further divide themselves into four spermatids, which have unique chromosomes that are half in number to the original spermatogonium.
- Stage 4: These cells now move through the lumen of the testes to the epididymis, where they mature into four sperm cells by growing microtubules on the centrioles, forming an axoneme, i.e., a basal body, and some of the centrioles elongate to form the tail of the sperm, facilitated by testosterone.
It is important to note that each division in the process is incomplete, and that the cells are always attached to each other by cytoplasm to allow them to mature at the same time. Also, some spermatogonia replicate themselves, rather than change into spermatids, which ensures that the supply of sperms does not run out. Throughout the entire process, spermatogenic cells interact with sertoli cells, which provide nutrition and structural support to them.
Factors Affecting Spermatogenesis
- The process of spermatogenesis is very sensitive, and can be affected by the slightest change in the levels of hormones such as testosterone produced by the hypothalamus, pituitary gland, and Leydig cells.
- The process is also very sensitive to changes in temperature.
- Deficiencies in diet, exposure to strong drugs, alcoholism, and presence of diseases can adversely affect the rate of sperm formation.
- Stress of oxidation can cause DNA damage to the sperms, leading to problems in fertilization and pregnancy.
The process of spermatogenesis in humans transpire over a time period that is more than two months long. During this time, over 300 million spermatozoa are produced on a daily basis. However, by the end of the process, only around 100 million become mature sperms. It can take another month to transport the new sperms on the ductal system.